Menopause is a natural stage of life that every woman will experience. However, while it is often associated with hot flushes and mood changes, its impact on pelvic health is less frequently discussed. Hormonal changes during menopause can affect the bladder, bowel, pelvic floor muscles, and sexual function — but effective, evidence-based support is available.
A pelvic health physiotherapist, regularly supports women through perimenopause, menopause, and postmenopause. With the right guidance, this transition can be managed confidently and proactively.
What Happens During Menopause?
Menopause is confirmed after 12 consecutive months without a menstrual period. It typically occurs between 45 and 55 years of age and includes three phases:
● Perimenopause – The transitional years when hormone levels fluctuate
● Menopause – When periods have stopped for 12 months
● Postmenopause – The years following menopause
During these stages, oestrogen levels decline. Oestrogen plays an essential role in maintaining the strength, elasticity, and blood supply of the pelvic tissues. As levels reduce, changes in the pelvic floor and surrounding structures may occur.
Common Pelvic Symptoms
Women may experience:
● Urinary leakage (especially with coughing, laughing, or exercise)
● Urgency or increased frequency
● Recurrent urinary tract infections
● Vaginal dryness
● Pain during intercourse
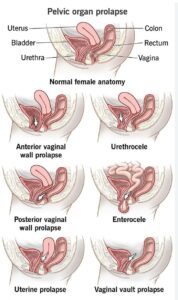
● A sensation of pelvic heaviness or prolapse
● Changes in bowel habits
These symptoms are common, but they are not something you have to accept as inevitable.
Why the Pelvic Floor Is Affected
The pelvic floor is a group of muscles and connective tissues supporting the bladder, uterus, and bowel. Reduced oestrogen can lead to thinning of tissues, reduced elasticity, and changes in muscle function.
Combined with factors such as childbirth, previous surgeries, chronic coughing, or high-impact exercise, menopausal changes can reveal or worsen pelvic floor dysfunction.
How Pelvic Health Physiotherapy Supports You
Pelvic health physiotherapy is highly individualised and goes beyond basic pelvic floor exercises. A specialist assessment allows us to understand how your muscles, breathing, posture, and daily habits interact.

During Perimenopause: Prevention
This is an ideal time for assessment. Early support can:
● Optimise pelvic floor strength and coordination
● Address early bladder symptoms
● Guide safe exercise and impact training
● Improve core and breathing mechanics
Proactive care can prevent symptoms from progressing.
During Menopause: Symptom Management
If symptoms are already present, treatment may include:
● Personalised pelvic floor strengthening or relaxation programmes
● Bladder retraining strategies
● Prolapse management
● Advice on vaginal moisturisers and when to discuss topical oestrogen with your GP
● Pain management strategies
Postmenopause: Long-Term Health
After menopause, maintaining pelvic floor strength is part of overall musculoskeletal health. Physiotherapy supports:
● Long-term continence
● Safe participation in strength training and sport
● Sexual comfort
● Core stability and posture
A Holistic Approach
Pelvic health does not exist in isolation. Sleep, stress, bowel habits, exercise, and breathing patterns all influence symptoms. A specialist physiotherapist considers the whole picture and creates a tailored plan based on your individual needs.
When to Seek Help
Consider an assessment if you experience leakage, urgency, pelvic heaviness, pain during intercourse, recurrent infections, or concerns about exercise. Equally, you do not need to wait for symptoms — preventative assessment can be extremely valuable.
Menopause is a significant life transition, but it does not have to compromise your comfort or confidence. Pelvic health physiotherapy offers practical, evidence-based support at every stage / helping you remain active, strong, and in control throughout menopause and beyond.
You can book an appointment now