You feel a pain on the bottom of your heel? It’s harder and harder to take your first steps in the morning and to walk for long hours? Your plantar fascia could be the cause.
You may already heard about plantar fasciopathy or jogger’s heel, but no worries, these differents terms describe the same thing: An irritation/inflammation of the plantar fasciitis: it’s an overuse trauma leading to micro-tears of the underneath of the foot.
To make it simple, your foot suffer from excessive load which damage the aponeurosis (sheet of flat tissue). The plantar fasciitis could be associated with a heel spur or not, but the treatment stays the same.
This injury is common among runners, but everyone can be affected!
What is plantar fascia?
The plantar fascia is a thick band of tissue on the bottom of your foot, that runs from your calcaneum (the bone of your heel) to your toes and constitute your arch foot.
Its role is to absorb shocks and support the arch to avoid the falling/flattening of the foot. Hence, we must take care of it, especially as we need our 2 feet every day!
While there is a relationship between the calf muscles, the Achilles tendon and the plantar fascia meaning this system muscle/ tendon/ fascia works together. Still this fascia is not elastic and when there is too much load on the foot, the plantar fascia becomes irritated leading to micro-tears.
What are the symptoms of Plantar Fasciitis? How to recognize a plantar Fasciitis?
The diagnosis of plantar fasciitis is based on a physical examination. The symptoms are the followings:
- Pain on the bottom of your heel, which can move under the foot.
- It’s a sharp and acute pain (sometimes a burning pain) which generally appear progressively.
- The pain is usually worse in the morning, when going out of bed: no doubts, the first steps remind you the pain is here! It takes several minutes to walk properly. As well, pain can appear after a long period of rest (at the moment, because of the home office, you can feel the pain when getting up after long hours of sitting).
- The pain worsens when weight-bearing, walking, or staying standing
- The pain eases with rest or if you avoid putting weight on your heel. You prefer walking on the ball of your feet? It’s probably time to see a doctor or a physio!
- In most cases, the pain affects just one foot although it can affect both (in which case it’s necessary to dismiss a potential rheumatic pathology)
If all these symptoms speak to you, you probably wonder why your plantar fascia cannot support as many load as it should?
What are the causes of Plantar Fasciitis?
First, there are « biomechanical » causes such as:
- An unusual excessive load (increase number of training sessions, change of work station, change of training surface, etc.)
- Feet posture: Flat feet/ high arches or a feet that collapse inwards
- Weakness of the calf muscles and foot muscles
- Tightness of hamstrings, Achilles tendon and calf muscles (remind you : the relationship between the plantar fascia and the calf)
- Loss of foot mobility or an unstable ankle.
In addition, there are more « global factors » that must be considered:
- Overweight
- Running and high-impact sports (Basketball, Handball, etc.) orif you have recently started exercising that you were not used to (The resolution to start brisk walking during the lockdown for example)
- Age: loss of the fat padding of the foot
- Working on your feet all day
- Improper footwear. It’s time to change your shoes!
- Some treatments or diseases (such as: long term antibiotics/ diabetes)
- Bad lifestyle (diet, hydratation, sleep, etc.)
What are the treatments of Plantar Fasciitis?
The treatment is divided into 2 stages: One stage of pain management and one stage of reloading.
As soon as symptoms appear, triggering factor(s) should be removed. This can be achieved by reducing the excessive load: it will not be the same for a runner training for the marathon than for a sedentary person. For example, by changing your training plan or reducing your walking time, while doing none weight bearing activities such as swimming or cycling. This is not a COMPLETE rest!
During the first stage, you can start strengthening your calf with isometric exercises.
- In front a wall, weight on your 2 legs, rise on the balls of your feet.
– Hold the position 45 seconds and rest 1min30
– Perform it 3 to 5 times, every day
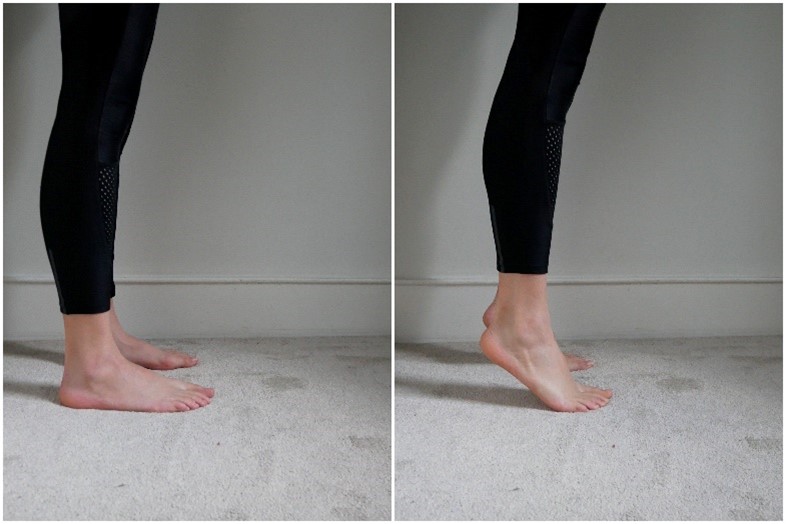
Once the pain has reduced you can continue the calf strengthening with eccentric exercises:
- Stand on a step with the balls of your feet on the edges, heels out of the step.
- Using both feet, lift on your heels and rise up onto the balls of your feet
- Slowly lower yourself as you wanted to « slow down » the descent until your heels are lower than the step (you should feel a calf stretch at the end).

You also can, every day:
- Massage the underside of the foot with ice cube
- Roll (see above) the underside of the foot over a small ball or with a frozen water bottle
- Stretch posterior muscles (calf and hamstrings)
- Strengthen your foot muscles (We’ll see it in more detail in a futur article)
For this last point, you can start by grasping the center of a towel with your toes (see below first photo). You also can try to lift your big toe while keeping the other four toes down and spread toes apart (see below second photo)
- Use gel heel pads: you should wear it every day for at least 3-4 weeks. (approx. 5mm, you can find it in sports shops). If that is not enough, you also can visit a podiatrist.
- Adopt a healthy lifestyle (sleep, hydration, diet)
Once the pain has reduced, it will be necessary to intensify the strengthening and progressively restarting to load the plantar fascia so that it readapt to the stress. (pas sûre de la tournure !)
How long does it take for plantar fasciitis to go away?
Unfortunately, it is difficult to say how long this will take, it varies greatly and depends on the severity of the injury. One thing is certain: the longer your pain has been there, the slower it will go away. However, don’t worry, it will eventually disappear.
Do not hesitate to visit a physiotherapist. They will be able to diagnose your problem, assist you for a progressive return to activity and put in place a specific treatment.
We can help you to restore the foot’s mobility by manual therapy techniques. The treatment may also include massage, stretching, K-taping, balance exercises and potential postural or sport gesture’s corrections.
For runners, we are also here to discuss with you the training plan you should follow or about your running form!