Main cause of Post Fall Syndrome: Frailty
Frailty is a common situation for people over the age of 65. It is characterised by a lack of adaptability and capacity to recover from external stress such as surgery, trauma or diseases.A more specific definition is: “A condition or syndrome which results from a multi-system reduction in reserve capacity to the extent that a number of physiological systems are close to, or past, the threshold of symptomatic clinical failure. As a consequence the frail person is at increased risk of disability and death from minor external stresses” (Partridge et al., 2012)
It is often associated with reduce muscle power, limited joint mobility, lack of stamina and motor function dysfunction which has a negative impact on other systems (cardiac, respiratory, etc.). Let’s see an example of vicious circle cause by frailty:An elderly person with postural disorder such as an increase kyphosis (a person with its back always bends forward) will have less mobility in its spine and ribs. This lack of rib cage compliance will lead to reduce breathing capacity then reduce stamina. Consequently, it will be more and more tiring for the person to perform his daily life activity such as going upstairs or walking.
However the most common and negative effect of frailty is the inability to recover from a surgery or a trauma and is often associated with a Post Fall Syndrome. Frailty can be managed and its consequence can be prevented with:- Exercise (Forster et al., 2010)
- Nutrition (Goodnough et al., 2011)
- Positive affect (Ostir et al., 2004)/depression (Billota et al., 2010)
- Psychosocial: social interaction (Lang et al., 2009)
Signs of Post Fall Syndrome
As mentioned previously, Post Fall Syndrome is composed of a combination of neurological signs, motor symptoms and psychological disorder:Motor symptoms
- Standing
- “Retropulsion” (gravity center kept backward)
- Posterior instability (tendency to fall backward)
- Both leading to postural compensation (Knees/hips kept flexed and bend forward) and to this traditional posture:

- Sitting
- Impairment of sitting posture is less visible but as problematic
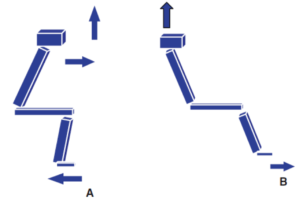
- Patients with PRS keep their buttocks forward, shoulders backward and feet far from the seat (image B)
- However, to stand up we need to transfer our gravity center forward (image A)
- Therefore, standing up is difficult/impossible without exterior help for patients with PRS (image B)
- Walking: it is difficult for them to
- Initiate the walk (they look like freeze)
- Difficulty to avoid obstacle and to turn
- Gait
- ↓ length of the step
- ↓ knees and hips flexion (↑ trip risk)
- ↓ heel strike
- ↑ time spend in bipodal stance (↑ posterior instability)
Neurological signs
- Alteration or absence of postural adaptation (the person is not able to balance herself and to stand up without falling)
- Protective reaction (put her arms in front when falling to slow the fall)
Psychological disorder
- Patient with PRS present with
- Anxiety/phobia of verticality (afraid to stand up)
- Loss of self-confidence/self-esteem
- Loss of motivation associate with a reduction of their activity and social interaction
- Therefore, they end up in a vicious circle
- They are afraid to move
- They move less
- They become even less able to move and even more afraid
Post Fall Syndrome Treatment: Walking rehabilitation
Walking is a natural activity for most of us. However, its apparent simplicity is only due to a constant training since a young age. In fact, walking is a very complex combination of movement involving muscles from all our body associated with constant stabilisations mechanism. Years of practice enable us to do it without thinking about it. Nevertheless, many causes can impair our walking. To restore a correct gait physiotherapy and a walking rehabilitation is often necessary. It combines:- Exercise to promote movement and strength
- Postural work to correct the compensation
- Work on the change of position to teach the easy and safe way to stand up, sit down, and lie down.
- Work on the walk and to correct their gait